Organs
Skin thickening is a common symptom in scleroderma, that is caused by scar tissue. In systemic sclerosis, this scar tissue or 'fibrosis' can become a very serious complication, as it forms within internal organs such as the lungs or the kidneys.
What causes the scarring?
In systemic sclerosis the immune system becomes overactive, causing the body to attack healthy tissues.
Part of the normal response of the immune system to deal with an injury or infection is to cause inflammation. When the immune system is overactive and continuously 'switched on', then this inflammation can cause damage to the body rather than healing it.
Normally, following an injury or infection, inflammation helps the body to repair itself by triggering the process of healing. For a more serious injury, part of the healing process involves scarring. In systemic sclerosis, excessive and continuous inflammation ultimately results in the development of scarring, or 'fibrosis'.
Kidneys
Although it is quite common for kidney function to be mildly reduced in scleroderma, this is not usually a major issue. If having scleroderma causes the kidneys to run at 50-70% of normal, this should still be sufficient for them to do their job adequately.
However, about 5-10% of people with systemic sclerosis (usually, but not only, those whose skin symptoms are worsening more quickly), will develop severe, uncontrolled high blood pressure from narrowed blood vessels within the kidneys. Over a short period of time, the narrowed blood vessels starve both kidneys of blood and oxygen, setting in motion the response of raised blood pressure. This eventually destroys the kidneys and damages the heart and lungs if left untreated.
This process is called scleroderma renal crisis. The symptoms of scleroderma renal crisis are:
- Very high blood pressure
- Severe headaches or blurred vision
- Breathlessness
- Nausea and vomiting
- Heart palpitations
- In some cases, seizures
Everyone with scleroderma renal crisis will initially need to be looked after in hospital. Some may require intensive care, coronary care or the specialist renal ward. Blood pressure medication will be given, and dialysis may be required if the kidneys have failed completely. People who do not recover after two years of dialysis may be candidates for a kidney transplant.
The heart
Heart disease becomes more common as we get older, so it is not surprising that it often occurs in people in their 50s and 60s who are living with scleroderma.
Systemic sclerosis can also directly impact upon the heart, so affected people are at greater risk of heart disease than others.
When heart disease is severe, the symptoms will be the same as for everyone else, involving breathlessness, chest discomfort, swollen ankles and palpitations.
Five common types of heart disease in systemic sclerosis:
- Coronary heart disease – systemic sclerosis may slightly increase your risk of developing the most common form of heart disease. Coronary heart disease causes angina, heart attacks and heart failure
- Systemic sclerosis heart disease is the most common type of heart disease directly caused by systemic sclerosis. Around one-in-ten patients with systemic sclerosis have high blood pressure in the lung arteries. This increases the work for the right side of the heart, causing it to thicken and eventually fail
- Valvular heart disease, especially aortic stenosis (narrowing of the main valve that controls blood flow leaving the heart for the rest of the body) is common in elderly people. It seems to be just as common in people with systemic sclerosis as everyone else. Symptoms are similar to coronary disease (above), although blackouts are more likely to occur
- Hypertensive heart disease – this happens when the heart has to work harder to deal with high blood pressure. The muscle of the heart is thickened, which can lead to rhythm problems (palpitations) and heart failure. High blood pressure affects nearly 50% of middle-aged people and is more common in systemic sclerosis because of kidney problems
- Rhythm problems - atrial fibrillation (a completely irregular heart rhythm) is one of the commonest rhythm disorders of elderly people, and tends to develop where there is fibrosis of the heart
Other heart problems that may arise:
- Pericardial effusions – this is a collection of fluid in the sac that the heart sits in. It rarely causes any problems. It can be due to inflammation of the lining of the pericardial sac or increased pressure within the heart (for example, when the heart is responding to high blood pressure in the lungs)
- Cardiac fibrosis or scarring of the heart muscle occurs in around one-in-five people with systemic sclerosis. Usually this is only picked up during scans, but very rarely it can become very severe and cause heart failure
- Small vessel disease - coronary artery disease affects the large vessels on the surface of the heart; in systemic sclerosis, the tiny vessels within the heart muscle also show abnormalities that are more prone to spasm and the failure to relax properly. This can cause very tiny areas of damage widely spread throughout the heart, which leads to a slightly weaker heart and slowed relaxation
- Myocarditis – sometimes inflammation occurs within the heart. Patients with myocarditis have symptoms of heart failure and rhythm problems. This can be identified fairly easily with blood tests and scans and treated with immunosuppression drugs

Heart Factsheet
Diagnosis and treatment
The diagnostic and treatment process for people with scleroderma is very similar to most heart patients.
Your doctor will take care during diagnosis to screen for pulmonary hypertension and any signs of thickening or scarring.
Any treatment that is needed should be managed in co-operation with a specialist who understands systemic sclerosis, so your cardiologist and rheumatologist will need to work together. This will help them get the balance right between treating the heart disease robustly and considering the complications of scleroderma.
Lungs
Up to half of scleroderma patients have some evidence of lung disease. Although the lung is often involved in scleroderma, not everyone will have symptoms suggestive of lung disease, so it is essential to identity this and begin treatment as early as possible.
Lung disease in scleroderma usually has a long, slow progression, so it is important to adjust to what you can and cannot do. It is advisable to do regular exercises if you can, and try to maintain a good basic level of physical fitness.
There are two forms of lung disease that are common in scleroderma:
- Pulmonary hypertension
Pulmonary hypertension is a rare lung disorder in which the blood pressure in the pulmonary artery rises above normal.
This happens in scleroderma when the blood vessels in the lungs narrow because of fibrosis, similar to the way that blood vessels to the fingers and toes are constricted in Raynaud's.
This abnormally high pressure affects the small blood vessels in the lungs, resulting in less blood reaching the lungs and less oxygen being carried into the bloodstream. As a result, the right side of the heart has to work harder to try and compensate for the blood vessels in the lungs.
Common symptoms include shortness of breath or feeling tired - especially on exertion or exercise, blackouts, and a very fast heart beat.
There are a number of ways of treating pulmonary hypertension, including with medication, oxygen, inhaled treatments and subcutaneous or intravenous infusions. There are also surgical procedures that may occasionally help.
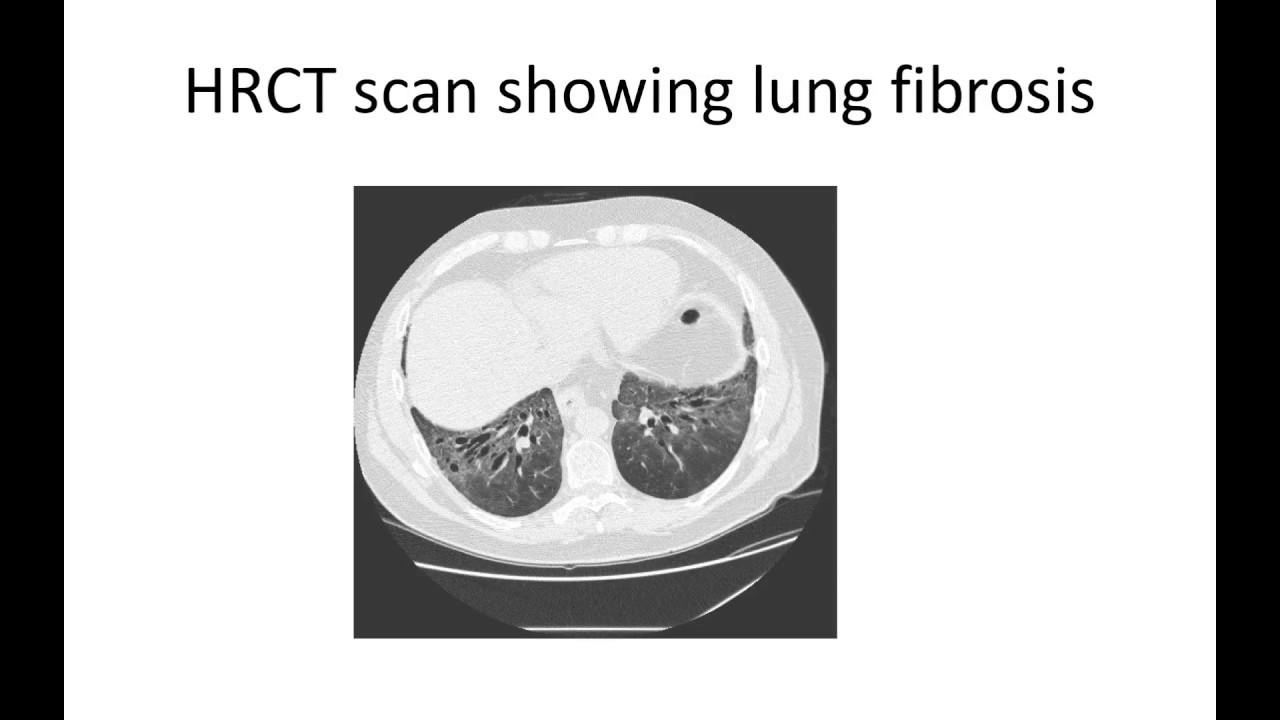
- Lung fibrosis
The earlier lung fibrosis is detected, the more likely there is to be a good response to treatment.
Fibrosis affects the alveoli, the tiny air sacs in the lungs. These are responsible for transferring oxygen from the air to the blood and removing the waste product, carbon dioxide, from the blood. The cells, which normally defend the body against infection, invade the lungs. While the scarring helps the injured areas to heal, it also results in thickening of the alveoli wall.
This means that the areas damaged by scleroderma fibrosis lose some of the elasticity and are therefore less able to perform their normal function. The body's cells that normally protect us from infection appear to be involved in the damage.
Breathlessness is the most common symptom, which may be noticeable when taking exercise or when walking up hills or upstairs. There may also be a dry, irritating cough.
Treatment of lung fibrosis is usually in the form of anti-inflammatory or immunosuppressant drugs, or intravenous treatments.
These need to be continued for as long as there is evidence of ongoing inflammation. For most people with systemic sclerosis and lung fibrosis however, it is usually possible to gradually reduce and stop treatment once the lung disease is no longer active. It is important to realise that this may take several years.