SRUK Research Sheds Light on the Effect of Calcinosis on Patients
Calcinosis is often a debilitating and painful symptom of systemic sclerosis. Last winter, SRUK led a piece of research in partnership with Professor Ariane Herrick, which aimed to build our understanding of the effect of calcinosis on people with scleroderma. We are thrilled to announce that the findings, which our community contributed to, have been published in the journal ‘Rheumatology.’ Read on to find out more about what we learned!
Calcinosis is often a debilitating and painful symptom of systemic sclerosis, that is thought to affect as many as 40% of people diagnosed. Calcinosis often causes physical impairment that in turn can have a considerable effect upon emotional wellbeing. Last winter, SRUK led a piece of research in partnership with Professor Ariane Herrick from the University of Manchester, which aimed to build our understanding of the effect of calcinosis on people with scleroderma. We are thrilled to announce that our findings from this research, which our community contributed to, were recently published in the journal ‘Rheumatology.’ Read on to find out more about what we learned from the research.
What is calcinosis?
Calcinosis cutis, or calcinosis for short, is a condition where insoluble calcium salts are deposited beneath the skin, which appear as chalky white or yellowish lumps. Calcinosis most commonly affects the fingertips, but can also occur on the knees, elbows, and face.
Calcinotic lumps are often painful, especially when they occur at pressure points. They can eventually break through the skin and cause ulcers, which may then become infected and require antibiotic treatment.
Although calcinosis is considered rare, it can affect between 20-40% of those living with systemic sclerosis and is more common in patients with the limited form of scleroderma. It is a neglected aspect of the condition as there is a lack of effective treatment options as well as limited documented evidence on how it affects the physical and mental wellbeing of those who experience it. Improving our understanding of these areas therefore has the potential to drive and inform more effective and tolerable treatments for people who are dealing with calcinosis as another part of their condition.
Our research and its findings: The SRUK Calcinosis Survey
The SRUK Calcinosis Survey was promoted through our social media channels. We invited our community to take part in this survey, covering various aspects including the areas of the body affected by calcinosis, the impact of calcinosis on day-to-day life, the treatments people have been prescribed and their levels of effectiveness.
Who responded?
138 people with scleroderma responded to our survey, with 129 people saying that they had calcinosis. As anticipated, most reported that they had limited systemic sclerosis (68%), followed by diffuse (22%), with the remainder either having localised scleroderma (4%) or being uncertain of their disease subtype (6%).
Which sites of the body are affected?
106 people completed all the survey questions, and their responses were included in the analysis of survey data.

Our survey confirmed that the hands and the fingers were the areas most affected by calcinosis, with 89% of our 106 respondents all reporting calcinosis at these sites. However, the data provided also showed that other areas were commonly affected as well, including the elbows (33% of people), the feet and toes (24%), the forearms (21%), and the knees (20%). Our survey also demonstrated that calcinosis may affect more than one part of the body, with 64% of people saying they experienced calcinosis at more than one site.
The impact of calcinosis on daily life
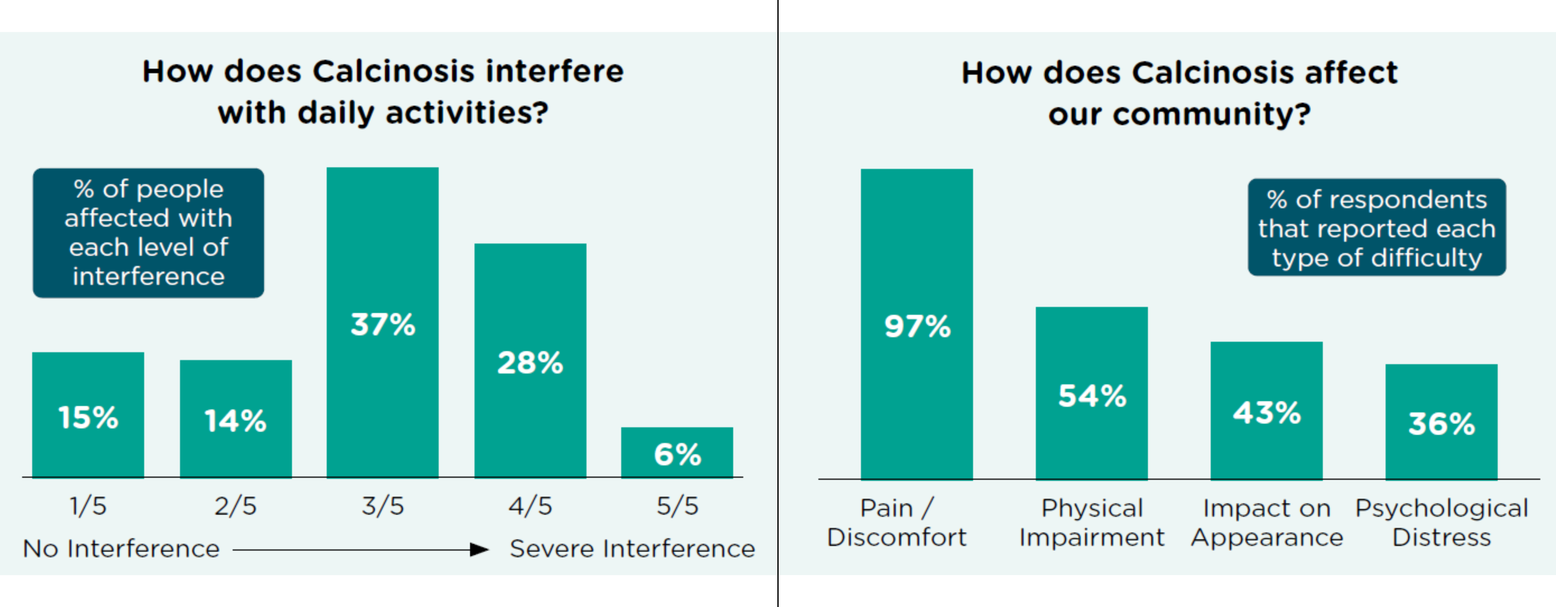
Seventy-one percent of those who responded said that calcinosis had a moderate-to-high negative impact on their daily life. The majority of respondents said that the calcinosis caused them pain and discomfort (97%) along with physical impairment (54%). This is perhaps linked to the high percentage of people (86%) who said that their calcinosis had ‘come out’ or broken through the skin causing ulceration that requires treatment with antibiotics.

Just under half of those affected (43%) said that calcinosis impacted upon their appearance. Given the wide range of effects mentioned above, it is perhaps unsurprising that just over one-third (36%) said that their experience of calcinosis had negatively affected their mental wellbeing and had caused them psychological distress.
Treatments and their effectiveness

Over half our respondents had not received any treatment for their calcinosis. Of those who did have treatment, a diverse range of medications had been prescribed including antibiotics that were presumably given for ulcerations that became infected. One-fifth of those who participated had received surgery to treat calcinosis. It was widely accepted among participants that the medication(s) they were prescribed were ineffective (90%).
How can this data help inform new treatments or better care?
The publication of the survey results in ‘Rheumatology’, a leading specialist medical journal, form a source of evidence which provides insight into the physical and mental burden of calcinosis on those with scleroderma, along with the need for more effective treatments. Clinicians, researchers and patient organisations like SRUK can point others towards this evidence, to show the burden that calcinosis places on individual patients and the healthcare system, to leverage funding for more research into calcinosis including new treatments, and to advocate for better care for these patients.
Where next?
Professor Ariane Herrick has a clinical interest in calcinosis, and in 2014 was awarded £111,268 by SRUK’s legacy charity the Raynaud’s and Scleroderma Association (RSA), for a three-year research project entitled ‘Novel Therapies for Systemic Sclerosis-related Calcinosis’. This funding enabled Professor Herrick to research the molecular aspects of calcinosis and identify compounds which could form the basis of a new topical treatment (something that could be applied directly to the skin of the affected area).
After completing the RSA/SRUK funded project Professor Herrick obtained another award from Versus Arthritis, to further test the compounds identified through the earlier project and how they should be formulated (i.e., as an ointment, gel, cream, or patch etc), to be applied to the skin.
Professor Herrick has identified a promising compound which she would like to study in a preliminary clinical trial, to test its safety and effectiveness in a small number of patients with calcinosis. Clinical trials are very expensive, requiring the input of the wider healthcare ecosystem, but Professor Herrick and Dr Mike Hughes are currently in the process of applying for funding from a large funder that can support studies of this kind. SRUK are also working with the team in our capacity as a patient organisation. We are delighted to play a role in the continuation of this story to a potential clinical trial, following on from the RSA’s initial seed funding which allowed the foundational elements of this research to take place. We hope that work like this, along with the findings of our survey, will lead to greater activity and better treatments for calcinosis in the future.
